Increased assisted reproduction and uterine surgery is leading to higher risk factors for women during and after birth. This includes Placenta Accreta Spectrum and the potentially serious sequalae. In this article Amisha Adhia, Founder, Action for Accreta and Miss Chineze Otigbah, Consultant Obstetrician & Gynaecologist highlight the issues around this condition and the role midwives may play in the multidisciplinary team to provide care and support.
Women’s Uterine Histories Have Changed and Our Awareness Needs to Keep Pace
Something has shifted in the last two decades that has quietly but significantly changed the risk profile of the women midwives care for every day.
Caesarean section rates in England have risen substantially, 45% as of NHS Data 2024-2025). Around 1 in 32 UK births result from IVF or assisted reproduction. Hysteroscopic surgery is more widely performed. Uterine curettage, for miscarriage management, or management of sepsis following miscarriage, or retained products is common across reproductive age groups. Endometrial ablation, myomectomy, and uterine artery embolisation are established parts of gynaecological practice. Hysteroscopic procedures to improve fertility, including removal of uterine septum or adhesions, are increasingly common. More women are entering pregnancy having had one or more of these procedures, and often more than one over the course of their reproductive lives.
Each of these interventions can alter the uterine environment in ways that increase the risk of placenta accreta spectrum (PAS), a condition in which the placenta fails to separate normally from the uterine wall, creating serious haemorrhage risk at birth. These are not marginal trends. They represent a meaningful change to the risk landscape that midwives are working within, and awareness needs to keep pace.
Current RCOG guidance, Green-top Guideline No. 27a, centres PAS risk primarily on prior caesarean section and placenta praevia (low-lying placenta). This leaves a significant population of women outside the thresholds that would typically prompt specialist referral: those whose uterine history involves curettage, hysteroscopic surgery, endometrial ablation, or other procedures, and those presenting without a low-lying placenta. Action for Accreta is calling for guidance to reflect the full range of risk factors the evidence now supports.
For midwives, the practical message is this: the guidelines do not yet tell the whole story. Clinical awareness and professional judgment remain the most important tools available in the meantime.
What Is PAS?
PAS describes a range of conditions in which the placenta abnormally adheres to or invades the uterine wall rather than separating cleanly after birth, from accreta (superficial attachment) through increta (invasion into the myometrium) to percreta (full invasion, potentially involving the bladder or bowel). The common thread is failure of normal placental separation, which creates significant haemorrhage risk at delivery.
When PAS is identified antenatally and managed at a specialist centre with a multidisciplinary team, outcomes are substantially better. The goal of earlier identification is simply to give more women, and their care teams, the opportunity to plan appropriately. A significant proportion of cases are still not diagnosed before delivery, meaning many women first encounter this condition as an emergency rather than a planned event.
Since 2020, PAS has been part of specialised commissioning by NHS England, with designated specialist centres providing diagnostic, neonatal, and surgical facilities for women with confirmed or suspected PAS. This infrastructure exists. The challenge is ensuring the right women reach it.
A Wider Risk Picture Than Many Midwives Have Been Taught
The traditional risk profile for PAS, anterior low-lying placenta in a woman with one or more previous caesarean sections, remains important. But it is incomplete.
Research demonstrates that a substantial proportion of PAS cases occur without placenta praevia. Work by Professor Daniela Carusi in the US has shown that more than 30% of confirmed PAS cases present without a low-lying placenta and that the majority of these women are not identified before delivery, in stark contrast to those with praevia-associated disease.
Studies present a mixed picture on clinical severity. Some, including Carusi et al (2020), found comparable rates of severe maternal morbidity between praevia and non-praevia cases, while others suggest non-praevia PAS may on average follow a milder clinical course. But this distinction risks obscuring what matters most for the individual patient. When non-praevia PAS goes undetected, as it does in the majority of cases, it does not present mildly. It presents as an emergency. The absence of antenatal diagnosis means the absence of preparation: no specialist team, no planned delivery setting, no informed consent. Whatever the population-level statistics show, the woman in that birth room faces the same haemorrhage, the same shock, the same loss of control. The clinical average is not the patient’s experience.
For midwives taking obstetric histories, this means looking beyond the caesarean scar question. A woman who has had previous uterine curettage, including following miscarriage or its complications such as sepsis, which may not always be fully recorded in a GP or maternity record, carries a different uterine profile than her records might suggest. Women who have undergone fertility treatment, hysteroscopic procedures, or prior manual removal of placenta may have sustained uterine trauma that never featured in a formal surgical record. For upper segment and atypical non-praevia PAS specifically, IVF conception, previous myomectomy, and advanced maternal age are recognised risk factors that warrant particular attention when taking a history.
This is not about interrogating women on sensitive histories. It is about holding a broader mental model of what “at risk” looks like, so that when a scan finding or a clinical instinct prompts a question, the right question gets asked.
What to Look For: Scan Findings at 12 and 20 Weeks
At the 12-week dating scan, PAS screening is not currently part of standard NHS protocol but early markers can be present and are worth noting, particularly in women with any relevant surgical history.
Features to look for include: low or anterior implantation of the gestational sac near a previous scar; loss or irregularity of the retroplacental clear space; increased vascularity at the implantation site on colour Doppler; heterogeneous or thinned myometrium beneath the placental site; and atypical sac morphology suggesting anterior wall embedding rather than normal endometrial implantation.
None of these findings constitutes a diagnosis in isolation. Their value is in prompting earlier conversation and follow-up.
At the 20-week anomaly scan, findings to discuss with the obstetric team include:
- Placental lacunae: irregular intraplacental vascular spaces giving a “moth-eaten” appearance; even lower-grade lacunae alongside a uterine scar are clinically relevant
- Focal loss of the retroplacental clear space: partial absence is as important as complete loss and more easily missed
- Myometrial thinning: less than 1mm beneath the placenta in the lower uterine segment
- Anterior placenta praevia overlying a uterine scar: this combination consistently warrants specialist review
- Bladder wall irregularity: any disruption to the normal echogenic bladder line
- Abnormal Doppler findings: bridging vessels, turbulent intraplacental flow, or uterovesical hypervascularity
It is also important to recognise that PAS is dynamic. The vasculature associated with abnormal invasion often does not become clearly visible on ultrasound until later in pregnancy, sometimes not until 28 to 30 weeks. A clear scan at 20 weeks can provide false reassurance while the condition continues to develop. Where risk factors are present, a normal anomaly scan is a reason for continued vigilance, not discharge from monitoring.
PAS can also attach in the upper uterine segment or fundal region, not only at the lower segment. Where location-based assumptions drive reassurance without full consideration of the woman’s uterine history, cases can be missed.
What Good Care Looks Like: Amisha and Louise
Amisha, who founded Action for Accreta alongside her husband Nik following their family’s experience of PAS, became pregnant with their daughter Ishaani in 2025. Her named midwife throughout was Louise Keane.
Louise holds a dedicated role as an abnormal implantation of placenta (AIP) midwife, a specialist position that mirrors, in its ethos and structure, the model many trusts will recognise from bereavement midwifery. The parallel is deliberate. Women with confirmed or suspected PAS are navigating one of the most anxiety-provoking diagnoses in obstetrics. They face a pregnancy in which the risks are serious, the pathway is complex, and the uncertainty can be profound. A named clinician who knows their case, holds their history, and is reachable when questions arise is not a luxury for this group of women. It is a clinical necessity.
Amisha’s case was assessed at five hospitals, including specialist PAS centres, before her condition was correctly identified. Her placenta was not low-lying, and without praevia her presentation did not fit the pattern that current screening pathways are built to detect. At each point, reassurance followed. It was only when she reached Barking, Havering and Redbridge University Hospitals NHS Trust (BHRUT), under the care of Miss Chineze Otigbah, that her PAS was recognised and a proper plan put in place. What made the difference was not just clinical expertise, but continuity. Louise’s consistent presence throughout, her knowledge of Amisha’s full history, and the integrated MDT structure meant nothing was lost between appointments, specialties, or shifts.
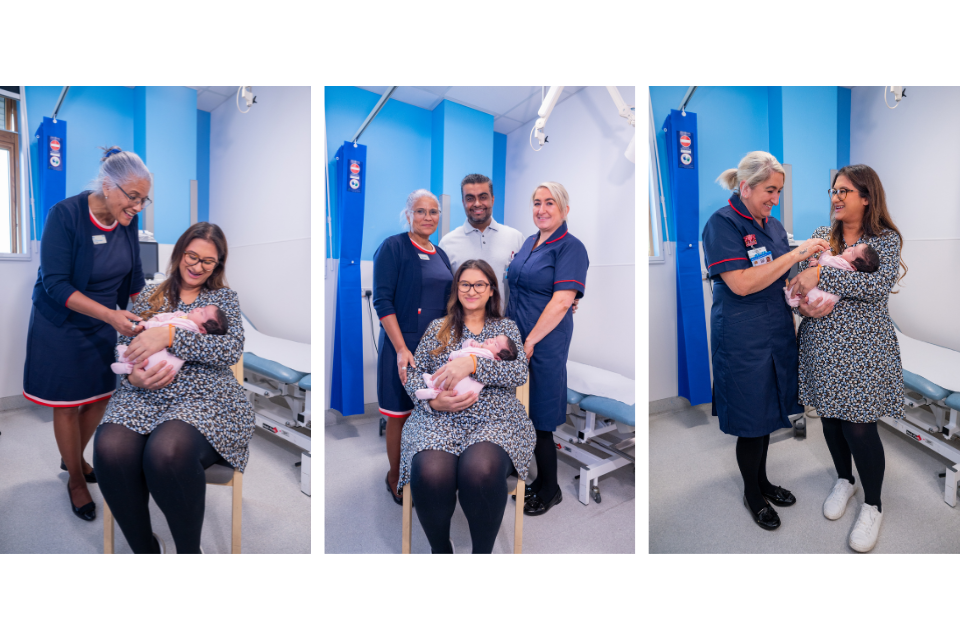
What this model offers goes beyond emotional support. Women with PAS require multidisciplinary planning that spans obstetrics, radiology, anaesthetics, neonatology, and often urology or interventional radiology. That planning has to be coordinated, updated as the pregnancy progresses, and held somewhere central. A dedicated AIP midwife organises and coordinates the MDT, representing the wishes of the woman and her family to the clinical team where required, and is present at those meetings as the woman’s advocate, ensuring her voice and full history inform every clinical decision. She supports skin-to-skin contact where it is possible, encourages feeding, and provides the reassurance that only someone who has been there from the beginning can give. Emergencies do not happen only during working hours, and a dedicated AIP midwife provides the connective tissue between specialties, the point of contact when concerns arise out of hours, and the person who already knows the woman’s situation when she calls.
The role does not end at delivery. Women who have experienced PAS face elevated risks of post-traumatic stress disorder and significant psychological sequelae. A dedicated midwife who has been present throughout is uniquely placed to monitor mental health in the weeks and months that follow, to recognise when a woman is struggling, and to ensure she is connected to appropriate support before crisis point. Risk identification also extends backwards: a thorough history, including screening for previous myomectomy, a significant but frequently overlooked risk factor for PAS, is part of what a specialist in this role brings to every case.
Not every trust currently has this role. Where it exists, it makes a measurable difference. Where it does not, midwives supporting women with complex placental presentations can still apply the same principle, ensuring there is a named person, a documented plan, and a clear escalation route within whatever structures are available.

When to Escalate: A Practical Guide
Discuss urgently with the obstetric team when:
- Placenta praevia is present, particularly anterior, with a uterine scar
- Any sonographic feature suggestive of PAS is identified at either scan
- Scar pregnancy is suspected at 12 weeks
- Antepartum haemorrhage occurs in a woman with a known uterine scar
Raise with a senior colleague or obstetrician when:
- A woman has two or more previous caesarean sections, even with a normal anomaly scan
- Any previous uterine surgery, including curettage or hysteroscopic procedures, is present alongside an anterior or low-lying placenta
- A prior pregnancy was complicated by adherent placenta or manual removal
- The anomaly scan report notes any placental finding for follow-up, however minor
- Clinical instinct suggests something warrants a second opinion
Document any concerns raised, including the clinical response. This supports continuity of care and ensures nothing is lost between contacts.
What Is Changing and How to Stay Informed
Action for Accreta is continuing to push for updated clinical guidance that reflects the full range of uterine risk factors, investment in specialist centre capacity, national coding and reporting for PAS, and dedicated midwifery roles of the kind this article has described. Our clinical resources, including the UK PAS Specialist Centres List are available here: https://www.actionforaccreta.org/nhs-pas-centre-list

About Action for Accreta
Action for Accreta is a national patient safety campaign founded by Amisha and Nik Adhia following their family’s experience of PAS. Since launching in February 2026, the campaign has documented the experiences of over 100 families, secured parliamentary engagement at the highest levels including cross-party coalition support from the former Secretary of State Sir Jeremy Hunt, Lord Hunt of Kings Heath (OBE), Helen Morgan (MP), and achieved the first dedicated questions on PAS in the history of Hansard, 18 in total since January 2026 revealing 9 government critical care gaps in England. The campaign has published the UK’s first publicly available PAS Specialist Centres List, supported by several leading maternal safety charities (Birth Trauma Association, Birthrights, Make Birth Better, MAMA Academy, White Ribbon Alliance UK, AIMS, Placenta Awareness UK, Delivering Better, and several others). They have also secured independent support statements from the Sands and Tommy’s Joint Policy Unit, whilst developing an economic case for earlier diagnosis and specialist-led care. The Track, Train, Trust framework sets out a practical roadmap for the infrastructure investment the condition demands.
We work alongside, not in place of, the clinical bodies and NHS organisations responsible for guideline development and service delivery. Our role is to ensure that the patient perspective, the evidence base, and the urgency of change remain visible.
You can find out more at: https://www.actionforaccreta.org/
Amisha Adhia, Founder, Action for Accreta & Miss Chineze Otigbah, Consultant Obstetrician & Gynaecologist
April 2026

