How much do you know about caring for people experiencing pregnancy and birth through a surrogacy arrangement? In this significant article, Gemma Cromwell, a third-year student midwife at The University of Bedfordshire, shares her personal experience, and those of others, to improve midwifery practices.
____________________
Surrogacy, what does that word mean to you on a personal basis? What thoughts does it bring to the forefront of your mind? To some people it may seem like an alien word – if you have not had any experience with the surrogacy world then that is completely understandable! According to the British Fertility Society, roughly 9% to 15% of couples will experience fertility issues and these issues can be for a multitude of reasons. There is also an increase in same-sex couples being able to achieve their dream of becoming parents due to ever-improving medical advances.
Anyone familiar with the Royal College of Midwives forum will have seen that recently there has been some online training on Surrogacy within the NHS. So, let’s take a quick look at what it means,
Surrogacy is the act of a birthing person carrying a baby for another person or couple. This can be as traditional surrogacy, (birthing a person’s eggs and the couple’s partner’s sperm), or gestational surrogacy (the egg and sperm from the couple). The baby must be genetically related to the intended parents (IP’S), either the person who requires a surrogate or one of the couple.
The purpose of this article, however, is not to inform on medical interventions to start what is known in the surrogacy world as a “journey” but rather the other end of the scale. Once a viable pregnancy has been confirmed, how is that journey through the National Health Service for these unique families?
A little about me! I am a mother of two children; I have at times in my past felt very lost and almost without purpose. When pregnant, I felt protective of the growing baby but when I saw my child and cradled them in my arms that is when I knew, THEY were my purpose. I looked on at the midwives who had supported me throughout my pregnancy with somewhat adoration – I felt that they had gifted me a new life, one as a mother. Roughly six weeks after the birth of my second child, my daughter I felt an immense sense of grief – I didn’t think I would be having any more children, but not only that, I grieved for the families who had never been fortunate enough to have that feeling of being complete. Of feeling whole. It prompted a lot of research into how I could help a family become just that… a family.
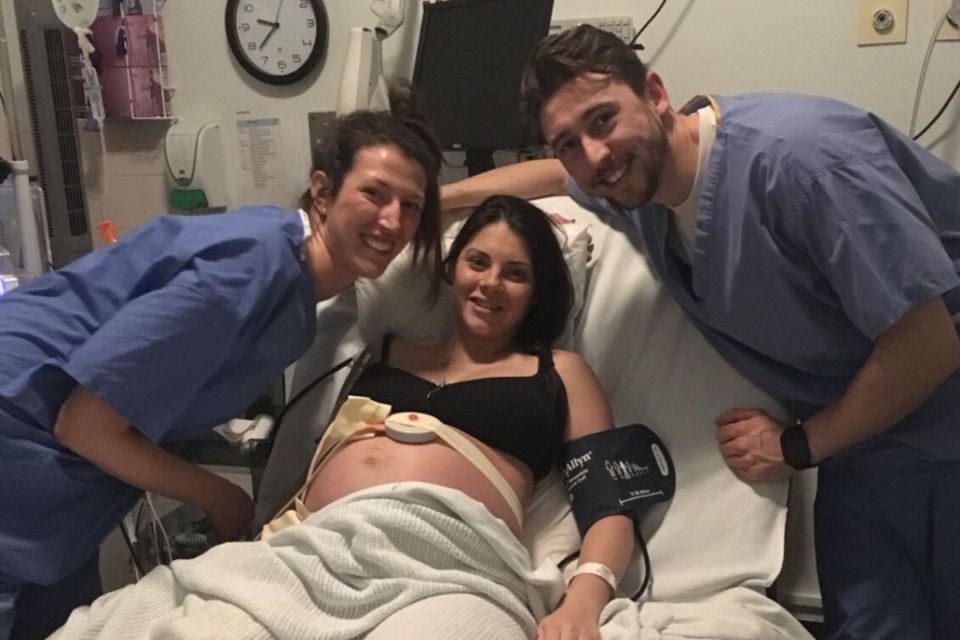
I met the most wonderful couple in 2016 and we clicked straight away; there are various protocols to go through during the “get to know period” including clinic visits, counselling, and legalities such as will writing and life insurance. Unfortunately, at the time British laws did (and still do) need updating and the parents-to-be would not be recognised as the official parents until the baby was born and at least six months old when a parental order can be granted by the courts. Due to this, we were understandably nervous about how our treatment might be at the hospital or by staff.
At every midwife appointment we were fortunate to have the same midwife, (beginning of continuity of care!): she was amazing.
- She directed questions about my personal and obstetric history to myself.
- When talking about the baby she spoke calmly and reassuringly to the parents.
- When she listened in for the fetal heart rate she involved the couple, asking if they would like to record the heart rate.
At ultrasound appointments:
- When appropriate, the screen was turned toward the couple so that they could see their baby and we were all treated with dignity and respect.
At the birth:
- We were all included in the discussion around the induction of labour.
- A meeting was held with the hospital representatives to understand who I would like in the labour room, for me to give permission for baby to stay with their parents after the birth and I documented permission for them to authorise any screenings, for example to hearing check and NIPE check, and finally to leave the hospital without me.
It must seem very weird to read it all so matter of fact; I thought it may help to understand the direct ways the hospital supported us and apply it to your own potential experiences within the trust. What isn’t so easy to put into words is the kind and considering nature of all staff, how nothing was too much for anyone. For example, the midwife who stood with the couple explaining what was going on in the labour room or the midwife who sat and held my hand and did breathing exercises when I entered a state of anxiety during contractions as I was labouring without my husband for the first time. I still remember to this day, feeling a contraction subside and opening my eyes to the calming eyes of the midwife; right there I knew at that moment this stranger was sharing my physical pain with me and it meant so very much. I don’t doubt at times I was probably the subject of gossip over a brew, but I was never aware of or felt any maltreatment.
It is important to note that, legally standing, my wishes and requirements as the birthing person would have been what is taken into consideration by health care professionals at the hospital. There have been instances where the birthing person and the intended parents have disagreed, and this can be very difficult for all involved. Trust’s will usually stipulate in their surrogacy policy that decision-making should be that of the birthing persons. In a surrogacy situation, the intended parent (s) and the surrogate mother should write an agreement and sign it together when they first match and prior to attempting pregnancy. It is not legally standing but it does ensure that both parties are on the same page around issues such as miscarriages, pre-term labour, and termination of pregnancies etc. The birthing person can stipulate who attends appointments, birth, and postnatal care of the baby. Ideally, if any areas are not in agreement, then they would “unmatch” early on because their ideals are not suited. This does not always happen and there may be instances that can be extremely emotional where extra verbal support and or legal support may be required or even safeguarding. You will need to refer to your surrogacy policy for guidance and may need to speak with a Professional Midwifery Advocate for support. Within my own “journey”, I stipulated for example that after the birth of the baby, the baby was to go straight to the intended parents while the cord was cut. I did not want to hold her in case I felt a rush of emotions. Throughout the pregnancy, if there was ever a decision to be made, we were all told together, and we discussed it privately and reached an agreement. I do believe communication is key – people may not always agree but we can compromise.
In the United Kingdom, you cannot be paid to be a surrogate, you can receive what is deemed by the courts as appropriate expenses for items such as travel, medical requirements, childcare etc. But if you ever hear a conversation around finances or the women in your care appears vulnerable or being taken advantage of, that concerns you, do not be afraid to raise your concerns with the appropriate person in your trust. Safeguarding those in our care must always be our priority if our instincts spike.
I have asked fellow surrogates for their reflections or a statement they feel would enhance our practice when supporting a surrogate pregnancy within the NHS – please be aware they will be anonymous to maintain confidentiality.
- Please remember for a lot of couples there has “usually been some kind of trauma (infertility/illness) that has led them to surrogacy”.
- Hospital surrogacy policy – Does your hospital have one and are you aware of it and what it includes? It is important to ask the surrogate mother what she would like to be referred to, calling her “mum” can be upsetting not only for the surrogate who has had counselling and knows that they aren’t mum, but also for the parents especially if they are present. Include the parents, involve them as much as you can, and ensure you read any birth plans for all eventualities including if a birth needs to be moved to theatre – who is coming to support the surrogate. Is everyone aware of what is happening and what consent is being given for?
- Skin to skin – for both my own experience and the surrogate who shared this with me; if the labourer does not wish for skin to skin then please offer the parents; they would love to offer the baby this warmth, and this opportunity for bonding is invaluable after the months of not being able to feel their own baby grow and wriggle. It can even be helpful especially if the labourer needs stitches!
- “A surrogacy champion – some trusts have lead specialists for LGBTQ, menopause, fertility or surrogacy”. This specialist can educate all clinical staff in appropriate and inclusive language to improve the birthing experience for all. Does your trust have this?
- One surrogate reflects that she had “two homebirths with surrogate babies”, the healthcare professionals “went out of their way to make the IP’S (intended parents) feel “part of a team” and able “to attend every scan, appointment, and consultation without hesitation and it was clearly documented” in the surrogate mother’s notes (remember always read all documentation and make your appropriate notes).
The key point to take away from this whistle-stop tour of being a healthcare professional involved with a surrogate pregnancy is: to involve not only the pregnant person but also the intended parent (s). Remember that extreme circumstances have brought these people together and you are another piece of that puzzle that is enabling a family to become whole, so treat everyone with kindness and respect. The law is not reflective of current situations and at times legalities can blur appropriate language for example, the surrogate may officially be the birthing person as they are the ones delivering the baby; however, ask the families how they would like to be referred to – document this in a place that other professionals will be able to refer to and address the families accordingly. A small gesture such as this will go a long way. Remember to check what your Trusts surrogate policy is and whether they have a surrogate lead and if they don’t and it interests you why not find out more information about becoming one yourself?
Let us all support inclusivity and adapt to the families in our care.
Gemma Cromwell, third year student midwife. University of Bedfordshire
March 2024


3 comments
I totally agree with everything you have said👍
Spot on.
I myself was a surrogate once(for a couple in Scotland and hD several files at ivf😭.
Shat made me decide or choose to be a surrogate.
Well when I was -8yrs old and got told I’d never be able to have kids naturally, because I’ve got PCOS.
Obviously this broke my heart😪.
Then three years later(surprise ) I found out I was pregnant with my first son. It had seemed the pregnancy had helped sort my body clock out after(started having monthly cycles)
3yrs later again, was pregnant with my eldest daughter.
I went onto have 2 more(4 kids I had altogether ).
I decided that I wanted to help other couples who are dealing with failed ivf treatment and broke there hearts(I knew how. they felt) because of my self (being told the same.
So I monteried my progestin track and learnt signs of when I’m near ovulation (as soon as I knew I was close to ovulation )
I called the couple down.Whilst me and the lady were talking, I gave her husband a sample pot.
He then passed the sample pot to me. I then did SELF Insemination in my bathroom.
3 weeks later I found out I was pregnant with the couples baby. When I informed all the professional that I was having a surrogate baby.
They all seem to be cross with me and disgusted(even my midwife) and others were saying I’m a baby seller😮🫣.
I was breaking the law , the said I’d be arrested, because it involves a lot of stuff Legally. Which I told professionals there was already a solicitor involved with the case. Which they didn’t seem to believe me😡.
Well they all got a shot, when they got a (photocopy) of the adoption order and me signing my parental rights onto the mother(she’s aged 13 now is there daughter)
I decided to do egg donation instead, after the experience
4 x I’ve done donation) now
Very interesting topic.
With so many mixed relationships surrogacy can become very challenging .
The challenges that I saw (public health role) is during
Baby Shower
27wk religious ceremonies (if Hindus)
and the role of the grandparents in this circumstances .
Interesting read.
I recently had the pleasure of performing the Newborn Examination of a baby who had the surrogate mother and the biological parents present
They were biological sisters who had done all the physical , emotional and legal journey together really well
It was important to preserve confidentiality when asking about medical history and regards consent to perform NIPE
They had such a good relationship and dyanamics between all 3 of them …. There was never any awckward moments.
The ward had accommodated all of them to stay together till discharged.
Comments are closed.