In this article Colm Darby, Advanced Neonatal Nurse Practitioner and Doctoral Fellow with the Neo-SILT Study at Queen’s University Belfast, explores the profound impact of neonatal admission on parents, highlighting how unexpected separation transforms a joyful milestone into a period of intense stress. Drawing on the Neo-SILT study, it identifies “Parental Role Alteration” as a primary stressor that disrupts early bonding. The piece advocates for trauma-informed care and better staff communication, emphasising that supporting parents’ roles is vital for family well-being throughout the neonatal journey.
For most parents, the birth of a baby is imagined as a time of closeness: a first cuddle, a first feed, the beginning of getting to know each other. For some families, however, birth becomes separation. Instead of staying together, parents find themselves watching their baby being transferred to a neonatal unit, trying to make sense of unfamiliar language, alarms, equipment, and the sudden loss of the beginning they had expected.
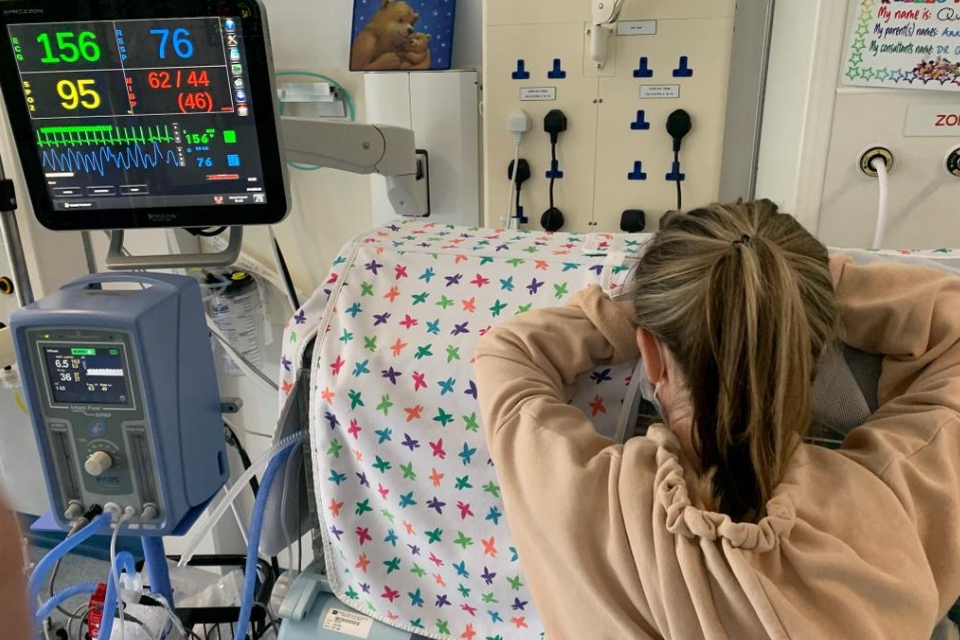
A neonatal admission is often necessary and life-saving, but for parents, it can also be one of the most stressful experiences of their lives. As healthcare professionals, we see that stress every day. We see it in the mother who is still lying in recovery, trying to understand what has happened while being told her baby has been admitted elsewhere. We see it in the father who is trying to hold everything together while worrying about both his partner and his baby. We see it in parents standing at the incubator side, overwhelmed, frightened, and unable to absorb information in the way they normally would.
That is why parental stress matters. It is not simply an emotional response happening alongside clinical care. It shapes how parents hear information, how they ask questions, how they make decisions, and how they begin to understand themselves in their new role as parents.
This was the focus of the work I recently presented at the National Maternity and Midwifery Festival, drawing on findings from the Neo-SILT study. Neo-SILT, which stands for Neonatal – Someone Is Listening to Trauma, is a Northern Ireland study exploring parental stress and trauma following neonatal admission. One part of the study examined parental stress using the Parental Stressor Scale: Neonatal Intensive Care Unit (PSS:NICU), a validated tool that looks at stress in three areas: Sights and Sounds, Baby Looks and Behaves, and Parental Role Alteration.
These areas tell us something important. Parents are not only stressed by the intensity of the neonatal environment. They are also stressed by what the admission does to their relationship with their baby and to their sense of themselves as parents.
In the Neo-SILT findings, parents were affected by the neonatal environment, particularly sudden monitor alarms and constant noise. They were also affected by their baby’s appearance and condition, especially signs of pain, tubes and equipment, unusual breathing, and the visible fragility of intensive care. But the strongest stressors overall were found in Parental Role Alteration. Being separated from the baby, feeling helpless, being unable to protect the baby from pain, and not being able to care for the baby in the way they had expected all scored highly.
Parents are not only distressed because their baby is unwell, they are distressed because neonatal admission can disrupt the very beginning of parenthood. It can leave them feeling that the role they had expected to step into has suddenly been taken from them.
The findings also highlighted differences between mothers and fathers. Both experienced significant stress during neonatal admission, but mothers reported higher stress across all three domains, with the largest difference seen in Parental Role Alteration. That does not mean fathers are coping easily or that their stress is somehow less important. In fact, fathers also reported substantial stress. What it does tell us is that fathers must not be overlooked, and mothers may be carrying an especially heavy burden where separation, helplessness, and disrupted expectations of parenting are concerned.
When stress was looked at across gestational age groups, parents of extremely preterm infants had the highest mean stress scores overall. The one area where gestational age made a statistically significant difference was the domain relating to the baby’s behaviour and appearance, suggesting that the visible fragility and medical complexity of very premature babies may be especially difficult for parents. Yet one of the most striking findings was that Parental Role Alteration remained high across all gestations, including term admissions. In other words, even when a baby is born at term, unexpected neonatal admission can still profoundly disrupt the parent’s early experience of bonding, caring, and being together.
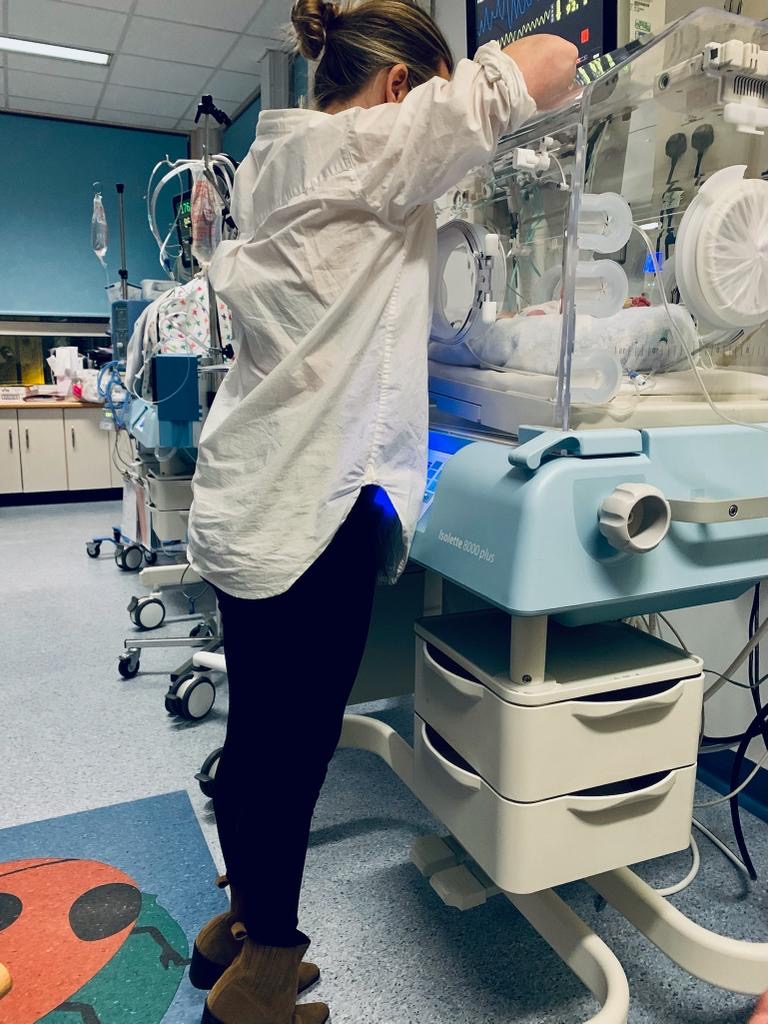
For maternity and neonatal staff, these findings are a reminder that family-integrated and trauma-informed care are not optional additions to good care. They are part of good care. If one of the strongest stressors is altered parenthood, then supporting skin-to-skin when clinically possible, involving parents in care tasks, explaining the environment, reducing avoidable separation, and helping parents feel that they still matter in their baby’s care are all deeply important. Parents need more than updates. They need help to feel close, included, and able to parent.
These findings matter for another reason too: high stress changes how parents function. A highly stressed parent may struggle to process information, ask questions, remember explanations, prioritise their own recovery, or cope with discharge while their baby remains in hospital. Parents may appear overwhelmed, detached, repetitive, or unable to make decisions in the way staff might expect. This is not poor coping. It is a predictable response to fear, uncertainty, and loss of control.
For maternity staff, this is just as important. Parental stress does not begin at the nursery doors. It often begins in labour ward, theatre, recovery, or on the postnatal ward, in the moment parents realise that their baby is unwell, being transferred, or will not remain with them after birth. Those early moments matter as they shape how frightened or supported parents feel, how much they can take in, and how they begin to make sense of what is happening.
This is especially true for fathers and partners. In urgent or emergency birth situations, particularly when caesarean birth is required, fathers may find themselves alone outside the theatre room while their partner is inside, surrounded by obstetric, midwifery, anaesthetic, and neonatal staff. They may be left waiting in a corridor with very limited information, worrying about the well-being of both their partner and their baby, only to be called in at the last moment for the birth itself. That period of waiting can be frightening and isolating. If the baby then requires neonatal admission, the father’s stress has not begun in the neonatal unit. It has already begun outside theatre.
For midwives, student midwives, and labouring support staff, this means communication is never just about relaying information. The words used during labour, birth, transfer, and the immediate postnatal period can either reduce or intensify distress. So can the actions that may seem small in the moment: preparing parents for what may happen next, explaining where the baby is going and why, including both parents in conversations, protecting opportunities for early contact where possible, and helping parents feel recognised as parents even when events are unfolding very differently from what they had hoped. Often, what families remember is not just the clinical event itself, but who noticed they were frightened, who explained things simply, who stayed, and who helped them feel less alone.
This is where the wider Neo-SILT study becomes so important. While these parental stress findings tell us a great deal about the immediate neonatal experience, they also raise a bigger question: what are the longer-term psychological effects of neonatal admission for parents? Neo-SILT is therefore continuing to explore post-traumatic stress disorder (PTSD) in parents across four timepoints over a 12-month period following neonatal admission. This will help us understand not only what parents experience in the early days, but how that experience may continue, change, or persist over time.
That matters because for some parents, neonatal admission does not end when discharge happens. It may continue in flashbacks, hypervigilance, avoidance, distress around anniversaries, or difficulty returning to the hospital environment. By following parents over time, Neo-SILT aims to strengthen the evidence base for earlier recognition, better support, and improved service planning for families affected by neonatal admission.
If Neo-SILT tells us anything clearly so far, it is this: parental stress is not only about what happens in neonatal care. It is also about what happens before neonatal care begins. Parents experience one journey across maternity and neonatal care, not separate professional boundaries. If we want to improve outcomes for babies and families, we must not only provide excellent clinical care, but also understand and respond to parental stress as a central part of that care.
Parents experience one journey across maternity and neonatal care; our task is to make that journey less frightening, less isolating, and more family-integrated from the very beginning.
Authors:
Colm Darby, Doctoral Fellow with the Neo-SILT Study at Queen’s University Belfast and an Advanced Neonatal Nurse Practitioner at Craigavon Area Hospital, Southern Health and Social Care Trust Northern Ireland.
Professor Olinda Santin, Queens University Belfast
Dr Derek McLaughlin, Senior Mental Health Lecturer- Queen’s University Belfast
Dr Breidge Boyle, Reader- Queen’s University Belfast
Corresponding author:
Colm Darby
07738174819
May 2026